Pharmacy Benefit Management
From transactional to transformational.
Our high-touch solutions help reduce spend, support better outcomes, and improve prescribing accuracy for injured workers.

Redefining the Role of Pharmacy Benefit Management
Filling the gaps, not just prescriptions.
We go beyond dispensing to identify risks, manage costs, and keep care on the right path.
More than a vendor
The oversight every decision should have.
A consistent team of CorVel pharmacists and certified pharmacy techs brings hands-on guidance and smart tools together to help reduce spend and improve oversight.
- One team driving smarter decisions across every claim
- Clinical oversight paired with intelligent pharmacy tools
- Always focused on both care and cost

Minimize support
Cost control that doesn’t compromise care.
From opioids to high-cost topicals, we look at the full picture to help employers reduce waste while making sure employees get what they need to recover.
- Convert expensive meds to affordable alternatives
- Promote generics where appropriate
- Actively manage opioid use and spend

Pharmacy insights
Full visibility across every pharmacy touchpoint.
Care🅪 connects the dots across your pharmacy data, making it easier to find gaps, control spend, and act before issues slow recovery.
- Track spend and utilization in real time
- Surface risks sooner with better insights
- Increase transparency with pharmacy claim oversight

Our solutions
Everything you need to get more from your pharmacy program.
Real savings, real impact
Reducing cost, risk, and unnecessary medications.
When pharmacy programs are aligned with care, it shows in the outcomes: lower spend, less opioid usage, and stronger savings across the board.
Saved per workers’ comp claim on average.
Reduction in total pharmacy spend.
Reduction in opioid day supply.
Care🅪
Our platform isn’t outsourced. It’s been strategically developed.
Care🅪 was built by CorVel for CorVel, shaped by decades of experience to give teams the insight, speed, and control they need to deliver better care and outcomes.
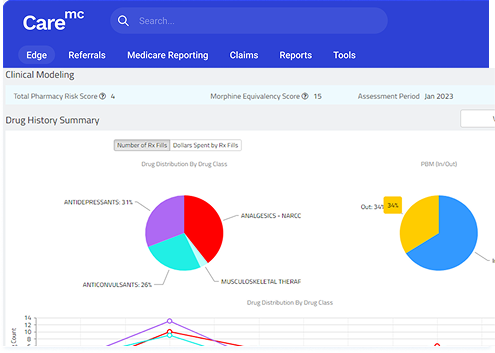
Helpful Insights
Let’s build what’s next, together.
Join the top organizations already partnered with CorVel.